Cataract Surgery
If a cataract makes it difficult for you to go about your normal activities or it interferes with the treatment of another eye problem, depending on the severity and progression of your cataracts, cataract surgery may be recommended to you.
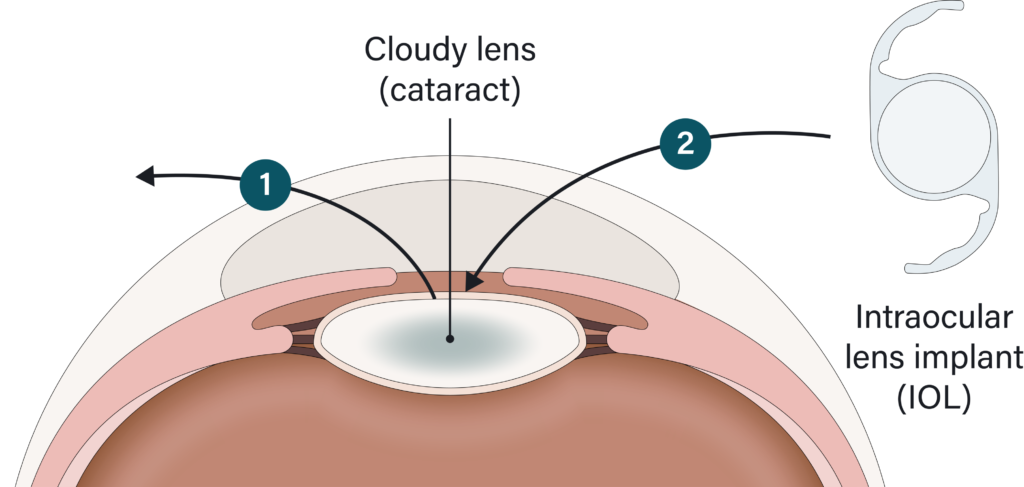
Cataract surgery is one of the most common surgeries performed and is a procedure to 1) remove the cloudy lens of your eye and 2) replace it with a clear artificial lens to restore vision. It’s performed on an outpatient basis which means you don’t have to stay at the hospital/clinic after the surgery and can go recover at home.
Because of the slow progression of cataracts, in most cases, waiting to have cataract surgery won’t harm your eye so you have time to consider your options and discuss them with Dr. Youssef. When considering surgery, ask yourself:
- Can you safely do your job? To drive?
- Do you have problems reading or watching TV?
- Is it difficult to cook, shop, do yardwork, climb stairs or take medications?
- Do vision problems affect your level of independence?
What to Expect
Before Surgery
Before surgery, Dr. Youssef will discuss your replacement lens options (IOL) with you and will measure your eye to calculate your chosen replacement lens power.
You must stop taking all medications at least 24 hours before surgery (including vitamins, supplements, and pain relievers).
Make sure you’ve arranged with someone to drive you after the surgery, because you’ll be going home the same day.
During Surgery
The entire surgery will take around 15 minutes to perform. Before beginning, you may be given a mild sedative to help you relax. Your eye is dilated with eye drops and the area is numbed with a local anesthetic. It’s possible that you might remain awake or drift off during surgery.
To remove your cloudy lens, Dr. Youssef with create incisions in the clear outer part of your eye (the cornea). The cloudy lens sits in a sac called the lens capsule, which he will open to be able to access the cataract inside the capsule. Once these openings are made, the lens can be removed by breaking it up with an ultrasound probe then suctioning it out like a vacuum. Once the cloudy lens is removed, your chosen IOL can be implanted into the now empty lens capsule.
When surgery is complete, a patch is placed over your eye as you rest for observation to make sure there isn’t any issues, such as bleeding or a reaction to the anesthesia.
After Surgery
Your eyes may feel itchy and uncomfortable for a couple days following surgery, but that’s normal. Absolutely DO NOT rub them for 3 WEEKS! It may result in SERIOUS complications and infections.
Dr. Youssef will schedule you for a follow-up visit the afternoon immediately following your surgery to ensure everything is healing properly, so head to PVSC if your surgery was at the Cornwall Community Hospital (CCH).
You will receive cards with the name and power of your lenses for your records. Hold on to them as we DO NOT keep copies at PVSC or CCH.
Keep your eyes closed for the first 2 hours (except to get around) after which you can remove the tape and start your drops. At the hospital you will receive a schedule for your eye drops (except if you’ve opted for dropless surgery). For bilateral patients, a prescription for two sets of eye drops is given for each eye. This is done for your own safety to reduce the risk of infection due to cross-contamination.
Your vision will be blurry for up to 24 hours after which most patients are able to drive. Physical effort like housework and working out are acceptable.
Colours will seem brighter because you’ve been looking through hazy/yellowish lenses for so long that you’re used to faded colours. You can anticipate some “floaters” but these will likely resolve within a few weeks.
Wear a protective shield for 1 week while sleeping and swimming goggles for 3 weeks while showering. We recommend you wear sunglasses outside for the first week for comfort and protection. You can purchase protective glasses, swimming goggles, and sleeping masks at PVSC optimized for post-surgical recovery.
During the healing process, use +2.00 or +2.50 reading glasses if needed until you see your optometrist for the final prescription. Advanced IOLs will make you less dependent on glasses but in the end, regardless of IOL choice, you may still need glasses for driving (mainly at night) and reading small print.
It is normal to see “quarter moons” or black blinders in the peripheral (side) vision due to the edge of the lens picking up extra light. Flickering will occur mostly when you go from a dark to light area or vice versa, but if they are present when your eyes are closed, contact PVSC as soon as possible.
Cataract surgery commonly causes dryness so use artificial tears 4 times per day if needed.
If you had dropless surgery, it is normal to see a white patch below the cornea under the lower lid. This can take a few weeks or months to go away.
If your vision does not clear within a few hours, if the vision worsens or you lose peripheral vision, or if you feel any pain or discomfort, contact us at PVSC. If it’s the evening or the weekend and you are having problems, you should go to emergency to be assessed.
What If My Vision Is Still Hazy After Surgery?
Your vision will probably be blurred for a short period following surgery, but then it should clear in an hour or two.
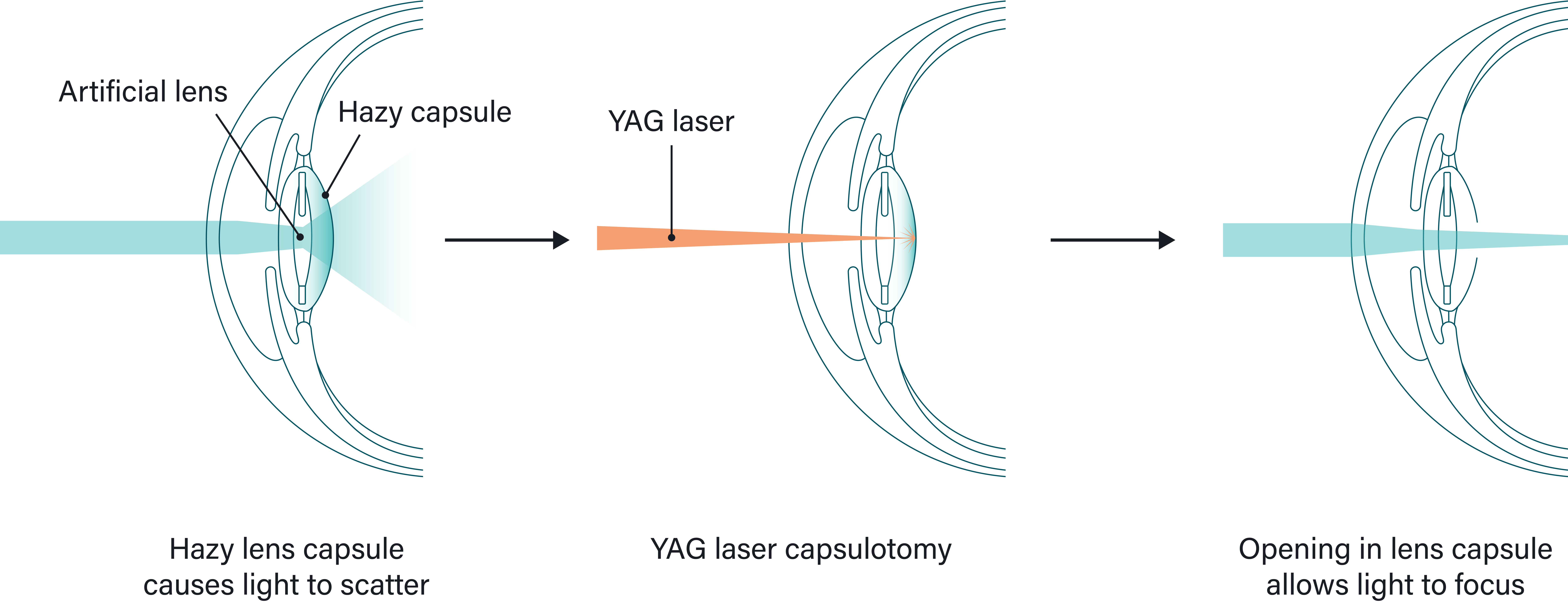
However, approximately 20% of cataract patients will develop haze on the membrane behind the IOL implant after cataract surgery making vision blurred/hazy (known as posterior capsule opacity). This can be fixed at PVSC by a quick procedure called YAG laser capsulotomy which uses a laser to create an opening in the capsule behind the IOL implant to allow you to see more clearly. The procedure is painless and usually takes 5 minutes so you’ll be able to go home soon after it’s done.
There are some rare risks with the YAG laser treatment such as inflammation, retinal detachment, lens dislocation, and raised eye pressure. Although uncommon, each of these problems is potentially serious. Rarely the procedure may need to be repeated.
Relax,you're ingood hands!
Risks
Cataract surgery is a common procedure and generally safe. For most people, surgery goes smoothly and they end up with better vision and recover without long-term issues. But like with any surgery, there are risks. We like patients to be aware of the possible complications of surgery so they can pay attention to any symptoms and inform us if something seems off.
Please be aware that your risk of complications increases if you have another eye disease or a serious medical condition. Sometimes, due to underlying eye damage from other conditions (like glaucoma or macular degeneration), cataract surgery can fail to improve vision. Dr. Youssef will discuss your options with you to determine the right steps to take.
It is imperative that you follow the post-op instructions listed above to reduce the risk of complications!
Intraoperative Complications
One of the risks during surgery is posterior capsule rupture/vitreous loss. The lens sits inside a capsule within the eye. Due to the nature of cataract surgery, this capsule may tear at any point during the operation. Loss of the vitreous due to capsular rupture can lead to severe visual disability and other complications such as retinal detachment.
Post-operative Complications
The most common complication of cataract surgery is dryness. The most serious complication is infection. To decrease risk of infection, Dr. Youssef injects antibiotics into the eye at the time of surgery which decreases the rate of infections by 1/7000. However, it is mandatory to avoiding rubbing the eye for weeks after your surgery as this introduces bacteria into the eye. It is strongly recommended that you wear an eye-shield for sleeping and sunglasses during the day for the first week following surgery. This decreases the chances of accidentally rubbing the eye and opening the wound allowing bacteria to get in.
Other possible complications after cataract surgery may include:
Surgery is performed under safe and sanitary conditions. Rarely, however, bacteria that get in the eye during surgery can lead to an infection, making you sensitive to light or have pain, redness, and vision problems. Infections after cataract surgery are rare (an incidence of 1/1000), but can be treated with an injection of antibiotics in the eye. In some cases, Dr. Youssef can remove the vitreous, the clear gel in the center of the eye, to stop the infection from spreading.
A little swelling and redness after surgery is normal. If you have more than usual, eye drops or other medicine can reduce inflammation.
After surgery, you have a slightly higher chance the retina pulls away from the back of the eye (retinal detachment). Retinal detachment is an emergency that could cause loss of vision so inform us immediately if you feel like a “curtain” has fallen over part of your eye, have new floating spots in your vision, and/or you see flashes of light.
When the cloudy lens is removed during surgery, some pieces may fall into your eye and get left behind. Small ones aren’t a problem, but bigger ones can be. You may need surgery to remove the vitreous and prevent swelling.
Sometimes after surgery, blood vessels in the retina leak. As fluid collects in your eye, it blurs your vision. This can be treated with eye drops and it could take weeks or months to heal. It usually gets completely better. In more serious cases, you may need a steroid shot behind the eye or surgery.
The artificial lens can slip out of place, causing blurred or double vision. It can also lead to more serious issues like bleeding and swelling. You may need surgery to get it back in position or to put in a new one.
In some cases, floaters have been there from before the surgery, hidden by the cataract. Once the cataract is removed, you may start noticing these floaters. The surgery can also cause posterior vitreous detachment, where the vitreous separates from the retina. It makes you see moving spider webs and clouds in your vision, along with flashes of light. Usually, it gets better on its own within a few months but because the symptoms are similar to retinal detachment, inform us right away to get checked out or head to emergency.
After surgery, if your vision is still cloudy, it is possible you’ve developed a secondary cataract, also called posterior capsule opacification (PCO). This is very common and can be fixed by a procedure called YAG laser capsulotomy in which a laser will create a hole in the back of the lens capsule to let light pass through so you can see normally.
The cornea is the clear, front part of the eye. It may get swollen and hazy after surgery making it harder to see. This problem is almost always temporary and gets better in days or weeks. It can be treated with eye drops.
It’s rare, but during surgery, blood vessels that supply the retina may start bleeding for no reason. A little bit of blood isn’t a problem, but larger amounts could lead to loss of vision. After surgery, blood may collect between the cornea and iris and block your vision. Eye drops may help, and you’ll need to rest in bed with your head up. If the blood doesn’t drain or causes too much pressure in your eye, you may need surgery.
For some people, surgery raises pressure in the eye (ocular hypertension). Dr. Youssef may suggest to treat it with eye drops, injections or medication depending on the cause (ex. swelling, bleeding, or leftover lens fragments). Frequent high eye pressure can damage your vision and result in glaucoma so it’s important to treat right away.
Light sensitivity is normal and expected and can be reduced by wearing sunglasses for a couple of months. If it lasts more than a couple of days, inform us immediately. It could also be a sign of another issue, like too much inflammation in your eye and may require eye drops.
This is a common condition after eye surgery. Doctors don’t know what causes it, but it typically goes away on its own. If it lasts more than 6 months, you may need surgery.
This causes you to see visual effects in two types:
- Negative: A curved shadow at the edge of your vision
- Positive: Halos, starbursts, flashes, or streaks of light
Doctors don’t know why it happens, and it often goes away on its own. It’s more likely to last when it’s the negative kind. You might need eye drops or even glasses with thick rims so you don’t notice the shadow as much. If it goes on for months, Dr. Youssef may suggest surgery. You might get a new lens or try a second lens on top of the first.
