Glaucoma
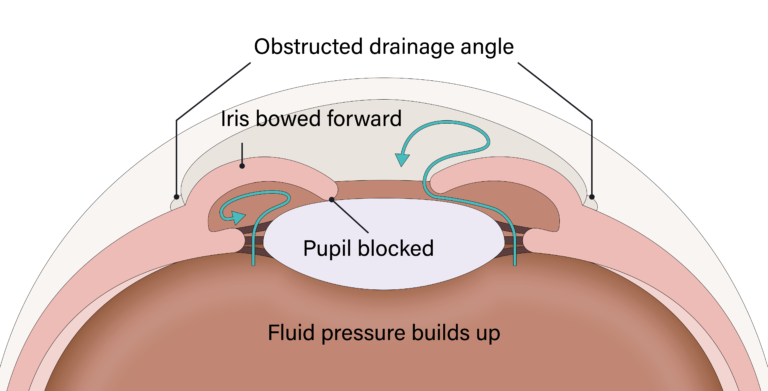
When light reaches your eye, it sends the signals to the brain to be turned into a visual image through the optic nerve. The optic nerve sits at the back of the eye and is similar to an electric cable made up of many wires. Any damage to the optic nerve can cause vision loss and blindness which is a disease called glaucoma.
A High Pressure Situation
High eye pressure alone doesn’t cause glaucoma but it is a significant risk factor.
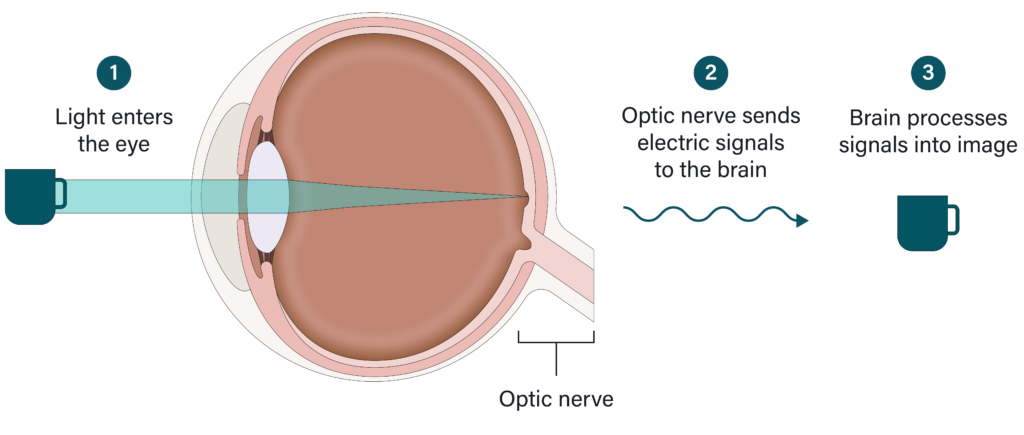
Your eye produces a clear liquid called aqueous humor. Its job is to circulate around the front part of the eye providing nutrients and giving it its shape. In a healthy eye, aqueous humor is constantly produced in small amounts at a time while equal amounts flow out. This is how your eye makes sure the pressure inside stays balanced.
Aqueous humor is produced in the back of the eye (posterior chamber) (1) then flows through the pupil into the front of the eye (anterior chamber) (2). It then flows out through a structure called the drainage angle (3) and drains into the eye’s circulatory system (4).
If the aqueous humor isn’t able to flow out properly, this can cause the pressure to rise higher than normal (think of a blocked garden hose). Fluid pressure builds up and causes damage to the blood vessels and optic nerve over time. If left untreated, this can cause blindness.
Glaucoma is considered to be the “silent thief of sight” because some people who have glaucoma aren’t even aware that they have it until it’s too late. When glaucoma develops, it’s difficult to detect early symptoms and the disease progresses slowly. Damage from glaucoma cannot be reversed which is why it’s important to be examined regularly to monitor and flag any changes to your eye health. Fortunately, early detection and treatment with eyedrops, surgery or both can help preserve vision.
Types of Glaucoma
Open-Angle Glaucoma
This is the most common form and occurs when the eye gradually becomes less efficient at draining aqueous humor. Typically, there are no symptoms in its early stages and vision seems normal but worsens as the optic nerve becomes more damaged causing large blank spots in the field of vision.
Half of patients with glaucoma don’t have high eye pressure when first examined so routine eye pressure testing and examining the optic nerve is important for proper diagnosis.
Closed-Angle Glaucoma
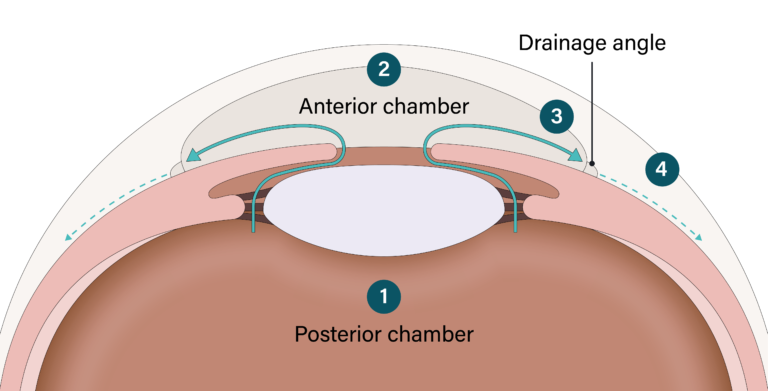
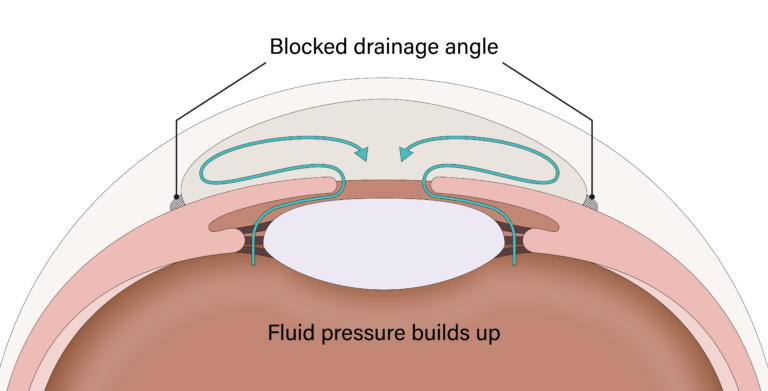
This is a less common form of glaucoma and occurs when the drainage angle of the eye is blocked. Unlike open-angle glaucoma, eye pressure usually goes up very fast. The pressure rises because the iris (the colored part of the eye) partially or completely blocks off the drainage angle resulting in a closed-angle glaucoma attack.
Symptoms of an attack include severe eye or brow pain, redness of the eye, decreased or blurred vision, seeing colored rainbows or halos, headache, nausea, vomiting. A closed-angle glaucoma attack is a medical emergency and must be treated immediately.
Other types of glaucoma include:
- Normal-tension glaucoma
- Congenital glaucoma
- Secondary glaucoma