Retinal Disorders
Posterior Vitreous Detachment (PVD)
The vitreous fluid is the gel-like, transparent substance that fills the space inside your eye. As you age, the consistency of the vitreous changes by shrinking or becoming more liquid. These changes can cause it to separate from the surface of the inside of the eye leading to a condition called posterior vitreous detachment (PVD). It can tug on the retina and peel it away from the tissue underneath causing a retinal tear. Left untreated, fluid can pass below the tear and behind the retina causing it to become even more detached resulting in a serious condition called retinal detachment.
PVD can cause visual symptoms such as flashes of sparkling lights (photopsia) when your eyes are closed or when you’re in a darkened room and new or different floaters may appear in your field of vision.
Retinal Detachment
When the retina, a layer of tissue at the back of the eye, pulls away from the layer of blood vessels below it, this is an emergency situation called retinal detachment. The blood vessels provide the retina with oxygen and nourishment so retinal detachment leaves the retinal cells lacking oxygen which itself is painless, but may cause you to lose vision in the portion of your field of vision that corresponds to the detached part. Early diagnosis and treatment can save your vision but the longer it goes untreated, the greater your risk of permanent vision loss in the affected eye.
Symptoms
Retinal detachment warning signs and symptoms almost always appear before it occurs or has advanced. If you experience any of the following symptoms, seek immediate medical attention:
- Sudden appearance of many floaters (small bits of debris in your vision that look like spots, hairs or strings and seem to float)
- Sudden flashes of light in the affected eye
- A shadow or “curtain” over a part of your vision that develops as the detachment progresses
Risk Factors
- Aging (more common in people over 40)
- Previous retinal detachment in one eye
- A family history of retinal detachment
- Extreme nearsightedness (myopia)
- Previous eye surgery such as a complicated cataract removal
- Previous severe eye injury or trauma
- Previous other eye disease or disorder
Treatment
If your retina has detached, Dr. Youssef can use surgical procedures to repair it. The specifics of your retinal detachment will determine which approach is best for you. Sometimes people need a second surgery for successful treatment.
Retinal detachment can be treated by:
Injecting Air Or Gas Into Your Eye
By injecting a bubble of air or gas into the eye, it floats against the retinal tear and the area surrounding the tear, it seals the tear. This stops more fluid from flowing into the space behind the retina. Fluid that had collected under the retina is absorbed by itself and the retina can then reattach itself to the back wall of your eye. You may need to hold your head in a certain position for several days to keep the bubble in place. The bubble eventually will also be reabsorbed on its own.
Indenting The Surface Of Your Eye
This procedure called scleral buckling involves sewing a piece of silicone rubber or sponge to the white of your eye (called the sclera) over the affected area. This causes the wall of the eye to indent which relieves some of the force caused by the vitreous tugging on the retina.
Draining And Replacing The Fluid In The Eye (Vitrectomy)
Draining the fluid in the eye (vitreous humour) is called a vitrectomy. Dr. Youssef will make a small incision in the eye to remove the vitreous humour then air, gas or liquids are then injected into the vitreous space to press against the retina causing it to reattach. Eventually the air, gas or liquid will be absorbed and your body will naturally refill the vitreous space.
A vitrectomy can be combined with a scleral buckling procedure.
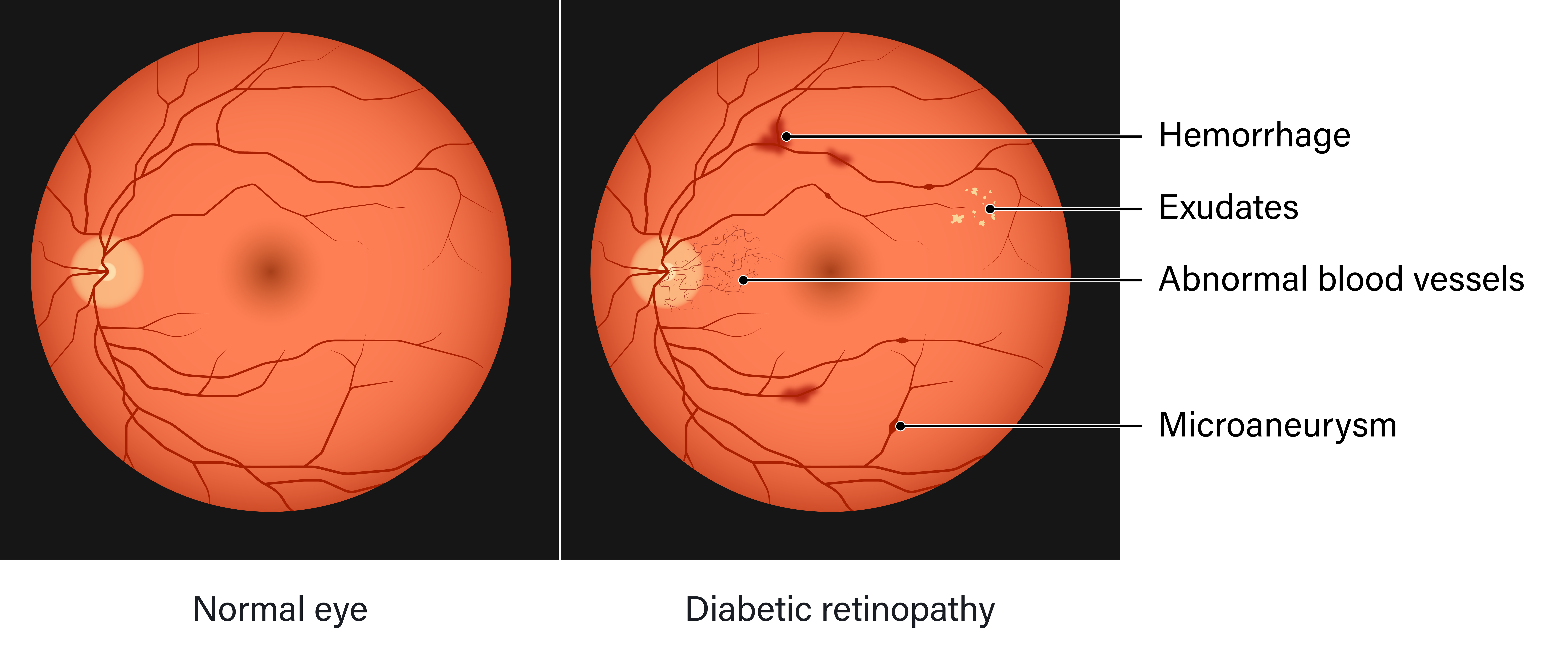
Diabetic Retinopathy
People with any type of diabetes can develop an excess of blood sugar and, although it’s an important source of energy for the body, too much of it causes damage throughout the body, including the small blood vessels in the eyes. Diabetic retinopathy is the most common diabetic eye disease and occurs when there’s a change in the blood vessels in the retina which usually affects both eyes. Sometimes these vessels swell and leak fluid or even close off completely. Other times abnormal new blood vessels grow on the surface of the retina.
People who have diabetic retinopathy often don’t notice changes in their vision in the disease’s early stages. But as it progresses, diabetic retinopathy usually causes vision loss that in many cases cannot be reversed.
There are two stages of diabetic retinopathy:
Nonproliferative Diabetic Retinopathy (NPDR)
This is the earliest stage of diabetic retinopathy when the walls of the blood vessels in the retina begin to weaken. This weakening can develop small bulges (called microaneurysms) which can leak fluid and blood into the eye.
The retina may also develop small deposits of cholesterol/fats from the blood that leaked (called hard exudates).
Areas of swelling in the retina (called macular edema) causes it not to function properly and is a major cause of vision loss in diabetes. When small blood vessels close (called macular ischemia), the retina isn’t receiving enough blood to work properly causing blurred vision.
While NPDR can cause vision problems, it doesn’t usually involve growth of new abnormal blood vessels on the retina. Once this occurs, it is a sign that the condition has progressed into the next stage of diabetic retinopathy called proliferative diabetic retinopathy (PDR).
Proliferative Diabetic Retinopathy (PDR)
When the small vessels in the retina close and the retina isn’t receiving enough blood flow, the retina attempts to fix this by growing new blood vessels (called neovascularization). Unfortunately, these new blood vessels are abnormal and don’t actually supply proper blood flow. This neovascularization is an indication that the condition has progressed into an advanced stage called proliferative diabetic retinopathy (PDR).
PDR is much more serious than NPDR because these abnormal blood vessels are delicate and bleed into the vitreous causing more visual problems like floaters or hazy vision.
New blood vessels also cause the formation of scare tissue on the retina. These wrinkles can distort vision or worse, can result in the retina getting pulled away from the back of the eye (retinal detachment) causing severe vision loss if not treated promptly.
Abnormal blood vessel growth can also occur in the iris (the colored part of the eye) which can block the flow of fluid out of the eye. Blocked fluid flow can cause the pressure to build up in the eye resulting in glaucoma (damage to the optic nerve).
Diabetic retinopathy takes years to develop which is why it’s important for patients with diabetes to undergo regular eye examinations and a yearly diabetic retinopathy screening. Detecting it in its early stages and monitoring the progression of the condition can help timely treatment to prevent vision loss.
Managing blood sugar levels, blood pressure, and other aspects of diabetes care is crucial in reducing the risk and progression of diabetic retinopathy. Advanced treatments may include laser therapy, intravitreal injections, and in some cases, vitrectomy surgery. At PVSC, we work closely with diabetic patients to develop and maintain an appropriate eye care plan.
Macular Pucker/Epiretinal Membrane (ERM)
A macular pucker (also called an epiretinal membrane) is a layer of scar tissue that grows on the surface of the retina, particularly the part of your eye responsible for detailed, central vision.
The macula is the small area at the center of the eye’s retina that allows you to see fine details clearly. The retina is a layer of light-sensing cells lining the back of your eye. As light rays enter your eye, the retina converts the rays into signals, which are sent through the optic nerve to your brain where they are recognized as images. Damage to your macula causes blurred central vision, making it difficult to perform tasks such as reading small print or threading a needle.
As we grow older, the thick vitreous gel in the middle of our eyes begins to shrink and pull away from the macula. As the vitreous pulls away, scar tissue may develop on the macula. Sometimes the scar tissue can warp and contract, causing the retina to wrinkle or become swollen or distorted.
The macula normally lies flat against the back of the eye. When wrinkles, creases or swelling affect the macula, vision can become blurry and distorted and you may even have a blind spot in your central vision.
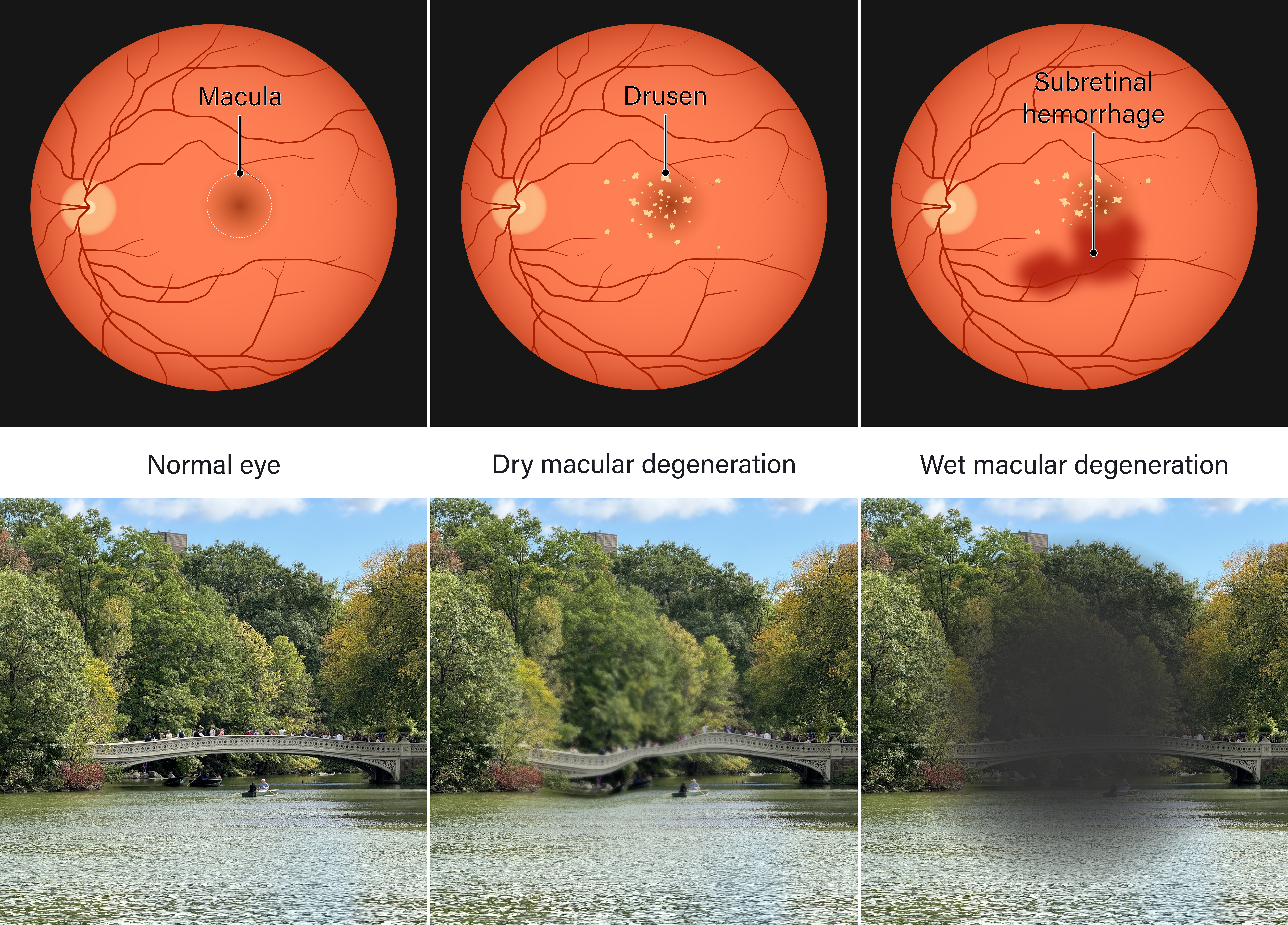
Age-Related Macular Degeneration (AMD)
Age-related macular degeneration (AMD) is a progressive eye disease that primarily affects older adults and can lead to significant vision loss. The macula is the central part of the retina responsible for sharp central vision, allowing us to see fine details and perform tasks like reading. AMD specifically affects the macula and can lead to central vision impairment while typically preserving peripheral vision.
There are two types of AMD:
Dry Type
Dry type is the more common form of AMD. Small yellowish deposits (called drusen) collect under the retina. This can affect the retinas normal function ultimately leading to the breakdown of photoreceptors in the retina (the cells responsible for detecting light).
As it progresses, patients with dry type AMD can experience increasingly blurred or distorted central vision.
Wet Type
Wet type is a more severe than dry type AMD because the abnormal blood vessel growth below the retina can leak fluid and blood. This leakage can cause quick and significant damage to the retina and central vision. Without timely treatment, this can result in severe vision loss.